People often start their journey to a healthier lifestyle by getting enough sleep, exercising, eating well, and taking mental breaks. Caring for teeth and gums? Not so much, which should change because preventing gum disease spells terrific news for your overall health.
Gum disease can lead to tooth loss. But research has also linked it to health problems, including heart disease, stroke, diabetes, and respiratory disease.
Check out below why you can’t underestimate proper dental care.
Gum Disease Causes
Gum or periodontal disease occurs when bacteria and plaque accumulate in the gums and the teeth, leading to infections and inflammation. The early stage is gingivitis, and you can reverse the damage at this point with dental treatment and proper oral hygiene.
However, if left untreated, gingivitis can progress to periodontitis, which goes deeper into the gums to affect the bone around the tooth. As a result, the gums can eventually pull away from the teeth, forming spaces called pockets that can become infected. Over time, severe cases of periodontitis can lead to tooth loss.
Gum Disease Symptoms
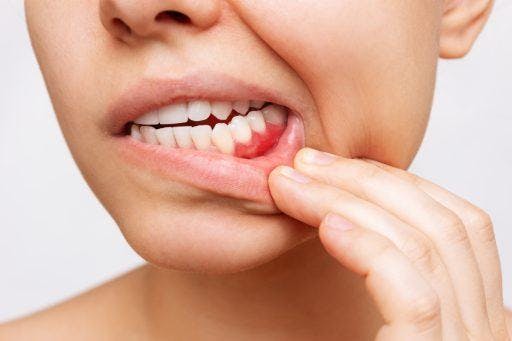
Regular dental checkups are essential because you may not see or feel any signs of gum disease until it’s too late. If you experience any symptoms below, see a dentist or periodontist for proper diagnosis and treatment as soon as possible.
Signs of gingivitis, the early stage of gum disease, include:
- Red, swollen, and tender gums
- Bleeding gums when brushing or flossing
- Bad breath or a bad taste in the mouth
The symptoms of periodontitis may include the following:
- Persistent bad breath or a bad taste in the mouth
- Receding gums or teeth that appear longer than normal
- Loose teeth or teeth that have shifted in position
- Pus between the teeth and gums
- Changes in the way teeth fit together when biting down
- Pain or discomfort when chewing
Impact of Gum Disease on Wellbeing

Inflammation puts the immune system on high alert, with implications that can affect the rest of the body.
For instance, research in Current Opinion in Rheumatology journal and by the National Rheumatoid Arthritis Society has shown that people with gum disease are at high risk of developing rheumatoid arthritis, which attacks the joints, and vice versa. In addition, the inflammation caused by gum disease can worsen the symptoms of rheumatoid arthritis.
In an interview, Dr Ron Ehrlich, a dentist and one of Australia’s leading holistic health practitioners, shares that a 62-year-old patient with rheumatoid arthritis could barely get up from the bed to walk to the bathroom for two years.
“His doctor thought maybe there was a dental connection, and there certainly was! He had advanced periodontal disease and a lot of dental infections,” Dr Ehrlich says, adding that the man did not have dental pain.
After recovering from his dental treatment, the patient not only could walk but he rode his bike to Sydney, Perth, and Melbourne.
Here are other health conditions associated with gum disease.
Diabetes
According to recent epidemiologic evidence, diabetes is two times more prevalent in patients with periodontitis than in those without. Saliva protects your mouth from dryness, food particle and bacteria build-up, and tooth decay. However, if you have diabetes, your body may not make enough saliva. On top of this reduced protection for your teeth and gums, diabetes can also increase the amount of glucose in your saliva. These problems can cause more bacteria to grow and plaque to build up in your mouth.
COVID-19
The SARS-CoV-2 virus primarily affects the respiratory system but can also cause inflammation throughout the body, including the gums. A 2021 study involving more than 500 patients found that people with periodontitis may be at higher risk of developing severe COVID-19 symptoms. In addition, COVID also increased the probability of assisted ventilation and ICU admission.
Cardiovascular disease
Research shows that people with periodontal disease risk developing atherosclerotic cardiovascular disease more than those with healthy gums. This is because the bacteria that cause periodontitis could enter the bloodstream and contribute to plaque formation in the arteries, narrowing blood vessels and increasing the risk of heart attacks.
Lung disease
Gum disease can worsen respiratory infections, such as pneumonia and chronic obstructive pulmonary disease (COPD). The bacteria that cause gum disease can travel from the mouth to the lungs and cause infections, especially in people with weakened immune systems or pre-existing lung conditions. Chronic lung inflammation can also weaken the immune system and increase the risk of gum disease.
Risk factors of gum disease
Aside from these health conditions, the following risk factors increase the chances of developing and worsening periodontal disease.
- Age 65 and above
- Poor nutrition
- Smoking
- Genetics
- Stress
- Medication (e.g., oral contraceptives and certain heart medicines)
- Grinding your teeth
Hormonal changes during pregnancy, puberty, and menopause can also make gums more sensitive.
Gum Disease Treatment and Prevention
Whether or not you have any risk factors, poor oral hygiene puts you at risk of developing gum disease. So preventive healthcare is still the best course of action. Start by developing these good dental hygiene habits.
- Brush your teeth at least twice daily and floss correctly. “Dry mouth” during sleep can cause tooth decay if you don’t brush your teeth before bed.
- Brush your teeth gently with toothpaste containing the recommended 1,350 to 1,500ppm fluoride.
- Use a soft-bristled toothbrush and pay extra attention to the three surfaces of your teeth: outside, biting, and inside surfaces.
- Visit your dentist regularly if you have crooked teeth, which can be challenging to clean properly. Your oral health provider may recommend removable aligners like ClearCorrect to straighten teeth. Dental aligners make it easier to brush and floss effectively, especially when tiny food particles get stuck between your pearly whites.
More serious cases of gum disease will require advanced treatment, including:
- Scaling and root-planing
- Antibiotic intake
- Tooth extraction
- Gum surgery
Consult with your dentist or general practitioner to determine the best plan for you. But ultimately, it’s all up to you to ensure you don’t take your oral health for granted and risk gum disease. Take a proactive approach to transform your smile today!
References:
American Thoracic Society. (n.d.). Dental Health and Lung Disease [PDF].
Asia, S. R. O. F. T. S. E. (2022). Action plan for oral health in South-East Asia 2022–2030. www.who.int.
Diabetes and Gum Disease Risk | ADA. (n.d.).
Gum Disease Risk Factors – American Academy of Periodontology. (2020, February 7). American Academy of Periodontology.
Ha, D., Spencer, A. P., Ju, X., & G, L., DO. (2020). Periodontal diseases in the Australian adult population. Australian Dental Journal, 65(S1).
Hirsch, R. (2004). Diabetes and periodontitis. Australian Prescriber.
Marouf, N., Cai, W., Said, K., Daas, H. I., Diab, H., Chinta, V. R., Hssain, A. A., Nicolau, B., Sanz, M., & Tamimi, F. (2021). Association between periodontitis and severity of COVID‐19 infection: A case–control study. Journal of Clinical Periodontology, 48(4), 483–491.
National Rheumatoid Arthritis Society (NRAS). (2022, November 10). Gum Disease link to rheumatoid arthritis (RA) | NRAS. NRAS.
Sanchez, P., Everett, B., Salamonson, Y., Redfern, J., Ajwani, S., Bhole, S., Bishop, J. A., Lintern, K., Nolan, S., Rajaratnam, R., Sheehan, M., Skarligos, F., Spencer, L., Srinivas, R., & George, A. (2019). The oral health status, behaviours and knowledge of patients with cardiovascular disease in Sydney Australia: a cross-sectional survey. BMC Oral Health, 19(1).
Sydney Holistic Dental Centre. (2021, July 20). How Gum Disease Can Affect Your Overall Health [Video]. YouTube.



